What is a Pragmatic Clinical Trial?
Section 2
The Embedded Pragmatic Clinical Trial Ecosystem
Definition of a Pragmatic Clinical Trial
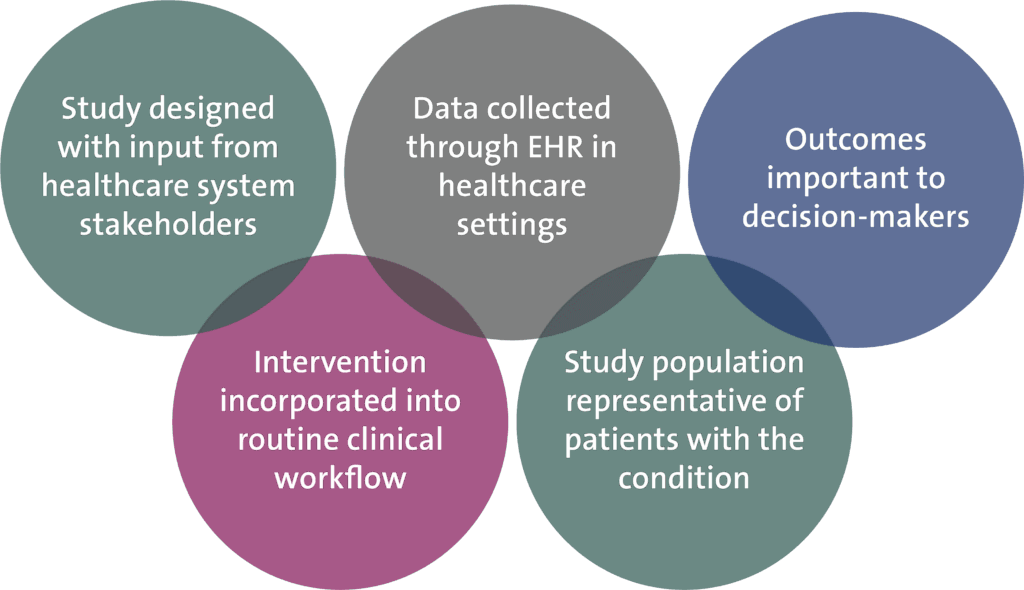
According to Califf and Sugarman (2015), there are 3 key attributes of pragmatic clinical trials:
(1) an intent to inform decision-makers (patients, clinicians, administrators, and policy-makers), as opposed to elucidating a biological or social mechanism; (2) an intent to enroll a population relevant to the decision in practice and representative of the patients or populations and clinical settings for whom the decision is relevant; and (3) either an intent to (a) streamline procedures and data collection so that the trial can focus on adequate power for informing the clinical and policy decisions targeted by the trial or (b) measure a broad range of outcomes. Given these attributes, a commonsense definition for a [pragmatic trial] would thus be as follows: Designed for the primary purpose of informing decision-makers regarding the comparative balance of benefits, burdens and risks of a biomedical or behavioral health intervention at the individual or population level.
Watch the video module: What Are Pragmatic Clinical Trials?
Bridging Clinical Care and Research
To produce generalizable results in an efficient manner, embedded pragmatic trials commonly take place in the settings where patients receive their usual care. In contrast with traditional randomized controlled trials, the intent in pragmatic trials is to avoid creating separate infrastructure with specially trained research staff responsible for data collection. For a broader, more representative study population, eligibility criteria in pragmatic trials are minimized and recruitment is expanded to all potentially eligible individuals receiving care in the participating setting. Intervention delivery, participant follow-up, and adherence protocols are more flexible and closely align with usual care to highlight the real-world implications of the intervention. These qualities of pragmatic trials lie along a spectrum of pragmatism, with some trials being more pragmatic than others (Thorpe et al 2009).
NIH Collaboratory Trials
To explore the potential of embedded pragmatic clinical trials and to establish best practices, the NIH Pragmatic Trials Collaboratory supports the design and implementation of the NIH Collaboratory Trials, which are embedded pragmatic clinical trials that address questions of major public health importance (Table) (Platt et al 2024).
Table. NIH Collaboratory Trials
| Trial | Goal | Population and Setting | Randomization |
| Completed Trials | |||
| ABATE Infection
Active Bathing to Eliminate Infection (NCT02063867) |
Evaluate the use of universal chlorhexidine bathing plus targeted nasal decolonization for hospitalized patients with methicillin-resistant Staphylococcus aureus outside the intensive care unit | 339,902 patients in 194 non–critical care units in 53 hospitals (Huang et al 2019) | Cluster randomization by hospital |
| EMBED
Pragmatic Trial of User-Centered Clinical Decision Support to Implement Emergency Department-Initiated Buprenorphine for Opioid Use Disorder (NCT03658642) |
Test the effectiveness of user-centered computerized clinical decision support on rates of emergency department–initiated buprenorphine/naloxone and referral for ongoing medication-assisted treatment in patients with opioid use disorder | 5047 patients with opioid use disorder under the care of 599 attending physicians in 18 emergency department clusters across 4 healthcare systems in 5 states (Melnick et al 2022) | Cluster randomization by emergency department |
| ICD-Pieces
Improving Chronic Disease Management With Pieces (NCT02587936) |
Improve care for patients with chronic kidney disease, diabetes, and hypertension by using a novel technology platform (Pieces) that uses the EHR to identify patients and by assigning practice facilitators within primary care practices or community medical homes | 11,182 patients with coexisting chronic kidney disease, type 2 diabetes, and hypertension in 141 primary care practices in 4 healthcare systems (Vazquez et al 2024) | Stratified cluster randomization of clinical practices within healthcare systems |
| INSPIRE
Intelligent Stewardship Prompts to Improve Real-Time Empiric Antibiotic Selection for Patients (NCT05423743 and NCT05423756) |
Improve physicians’ choice of antibiotics for patients hospitalized with abdominal, skin, or soft tissue infections by reducing unnecessary use of extended-spectrum antibiotics | 105,004 hospitalized adults with abdominal infection (Shruti et al 2025a) and 60,725 hospitalized adults with skin or soft tissue infection (Shruti et al 2025b) in 92 hospitals | Cluster randomized trial |
| LIRE
Lumbar Image Reporting with Epidemiology (NCT02015455)
|
Determine if inserting epidemiological benchmarks (essentially representing the normal range) into lumbar spine imaging reports reduces subsequent tests and treatments | 250,401 patients with low back pain in 98 clinics in 4 healthcare systems (Jarvik et al 2020) | Cluster randomization by clinic; stepped-wedge, one-way crossover design |
| Nudge
Personalized Patient Data and Behavioral Nudges to Improve Adherence to Chronic Cardiovascular Medications (NCT03973931) |
Use pharmacy refill data to test the effectiveness of medication reminder nudges delivered to patients’ mobile phones, and test an interactive chatbot mechanism that optimizes content | 9501 patients with chronic cardiovascular conditions who take medications in 3 large integrated healthcare systems (Ho et al 2025) | Individual-level randomization |
| PPACT
Pain Program for Active Coping and Training (NCT02113592) |
Help patients adopt self-management skills for chronic pain, limit use of opioid medications, and identify factors amenable to treatment in the primary care setting | 850 patients with chronic pain on long-term opioid therapy in 3 staff model health plans; 106 clusters of primary care providers (DeBar et al 2022) | Cluster-randomization by primary care provider |
| PRIM-ER
Primary Palliative Care for Emergency Medicine (NCT03424109) |
Test the effectiveness of primary palliative care education, training, and technical support for emergency medicine | 98,922 patients aged 66 years and older with serious life-limiting illness in 29 emergency departments (Grudzen et al 2025) | Cluster randomization; stepped-wedge design |
| PROVEN
Pragmatic Trial of Video Education in Nursing Homes (NCT02612688) |
Determine if showing advanced care planning videos in nursing homes affects the rates of hospitalization | 30,016 patients with comorbid conditions in 360 nursing homes (Mitchell et al 2020) | Cluster randomization by nursing home |
| SPOT
Suicide Prevention Outreach Trial (NCT02326883) |
Compare outcomes in patients who receive care-management or online skills training for suicide prevention versus usual care | 18,882 individuals at elevated risk for suicide in 4 large healthcare systems (Simon et al 2022) | Individual-level randomization |
| STOP CRC
Strategies and Opportunities to Stop Colon Cancer in Priority Populations (NCT01742065) |
Improve the rates of colorectal cancer screening by mailing fecal immunochemical testing tests to patients at federally qualified health centers | 41,193 adults eligible for colorectal screening in 26 federally qualified health center clinics in 8 health centers (Coronado et al 2018) | Cluster randomization by clinic |
| TiME
Time to Reduce Mortality in End-Stage Renal Disease (NCT02019225) |
Determine whether increasing hemodialysis session duration reduces mortality and hospitalization rates for patients receiving maintenance hemodialysis care | 7035 adults who had initiated treatment with maintenance hemodialysis within the previous 120 days in 266 dialysis units operated by 2 dialysis provider organizations (Dember et al 2019) | Cluster randomization by dialysis facility |
| TSOS
Trauma Survivors Outcomes and Support (NCT02655354) |
Coordinate care and improve outcomes for trauma survivors with post-traumatic stress disorder (PTSD) and comorbidity and to provide the American College of Surgeons with multisite pragmatic trial evidence that could further inform regulatory policy | 635 hospitalized adult survivors of physical injury with PTSD and comorbidity in 25 level 1 trauma centers (Zatzick et al 2021) | Cluster randomization by trauma center; stepped-wedge design |
| Ongoing Trials | |||
| ACP PEACE
Advance Care Planning: Promoting Effective and Aligned Communication in the Elderly (NCT03609177) |
Test whether clinician communication skills training and patient video decision aids increase completion of advance care planning | 13,800 patients aged 65 years and older with advanced cancer in 29 oncology clinics in 3 healthcare systems (Volandes et al 2025) | Stepped-wedge, cluster randomized trial |
| AIM-CP
Adapting and Implementing a Nurse Care Management Model to Care for Rural Patients With Chronic Pain (NCT06407115) |
Adapt and test a nurse care management model to provide comprehensive, coordinated care for patients with chronic pain in rural communities | Adults with chronic pain in primary care clinics in 6 rural-serving healthcare systems in 2 practice-based research networks | Type 2 hybrid effectiveness-implementation trial with individual-level randomization |
| APA-SM
Personalized Auricular Point Acupressure for Chronic Pain Self-Management in Rural Populations |
Test an auricular point acupressure intervention for self-management of chronic pain in rural communities | Adults with chronic musculoskeletal pain in healthcare systems serving rural communities in South Carolina and Texas | Type 2 hybrid-effectiveness implementation trial with individual-level randomization |
| ARBOR-Telehealth
Advancing Rural Back Pain Outcomes Through Rehabilitation Telehealth (NCT06471920) |
Test delivery of a telehealth physical therapy strategy to improve patient-centered outcomes and reduce opioid use among patients with chronic low back pain living in rural communities | Adults with chronic low back pain in primary care clinics in a healthcare system serving rural communities | Type 1 hybrid effectiveness-implementation trial with individual-level randomization |
| BackInAction
Pragmatic Trial of Acupuncture for Chronic Low Back Pain in Older Adults (NCT04982315) |
Evaluate the safety and effectiveness of standard and advanced courses of acupuncture in older adults with chronic low back pain | Adults aged 65 years and older with chronic low back pain in 4 performance sites | Individual-level randomization |
| BeatPain Utah
Nonpharmacologic Pain Management in Federally Qualified Health Center Primary Care Clinics (NCT04923334) |
Compare the effectiveness of nonpharmacologic interventions delivered via telehealth to improve pain management and reduce reliance on opioids for patients with chronic back pain in community health centers in Utah | Adults with chronic back pain in community health centers in Utah | Type 1 hybrid effectiveness-implementation trial with individual-level randomization |
| BEST-ICU
Behavioral Economic and Staffing Strategies to Increase Adoption of the ABCDEF Bundle in the ICU (NCT06184945) |
Build and evaluate behavioral economic and implementation science theory–based interventions fostering adoption of the ABCDEF bundle and improving clinical outcomes of critically ill adults | Critically ill adults on mechanical ventilation in 12 intensive care units in 3 hospitals | Stepped-wedge, cluster randomized trial |
| Chat 4 Heart Health
Using Artificially Intelligent Text Messaging Technology to Improve American Heart Association’s Life’s Essential 8 Health Behaviors (NCT06324981) |
Evaluate the implementation and effectiveness of 3 text messaging delivery strategies for self-management support to improve control of cardiovascular disease risk factors defined by the American Heart Association’s Life’s Essential 8 Health Behaviors | Patients in 3 federally qualified health centers | Individual-level randomization |
| FM-TIPS
Fibromyalgia TENS in Physical Therapy Study (NCT04683042) |
Test the feasibility and effectiveness of adding transcutaneous electrical nerve stimulation to nonpharmacologic treatment for pain and fatigue in patients with fibromyalgia | Approximately 6000 patients with fibromyalgia in 24 routine physical therapy clinics in 6 healthcare systems in rural and urban settings | Cluster randomization by clinic |
| GGC4H
Pragmatic Trial of Parent-Focused Prevention in Pediatric Primary Care: Implementation and Adolescent Health Outcomes in Three Health Systems (NCT04040153) |
Test the feasibility and effectiveness of implementing a universal evidence-based anticipatory guidance curriculum (Guiding Good Choices) for parents of early adolescents | 3 large integrated healthcare systems with 75 pediatric primary care practices serving 3600 families with adolescents aged 11 to 12 years | Cluster randomization by pediatrician within clinic |
| GRACE
Hybrid Effectiveness-Implementation Trial of Guided Relaxation and Acupuncture for Chronic Sickle Cell Disease Pain (NCT04906447) |
Determine the effectiveness of guided relaxation and acupuncture compared with usual care in reducing pain and opioid use for patients with sickle cell disease | Adults with sickle cell disease in 3 large healthcare systems | Cluster randomization |
| HiLo
Pragmatic Trial of Higher vs. Lower Serum Phosphate Targets in Patients Undergoing Hemodialysis (NCT04095039)
|
Test the effects of liberalizing the serum phosphate target (“Hi”) vs maintaining aggressive phosphate control (“Lo”) | Approximately 4400 patients with end-stage renal disease receiving maintenance hemodialysis at 100 sites in 2 large dialysis provider organizations | Cluster randomization |
| I CAN DO Surgical ACP
Improving Completion, Accuracy, and Dissemination of Surgical Advance Care Planning (NCT06090552) |
Use a model of expanded advance care planning as the foundation to support advance care planning engagement in older adults undergoing surgery | Patients 65 years and older, or with serious illness, who are referred for major elective surgery in 3 healthcare systems | Individual-level randomization |
| IMPACt-LBP
Implementation of the American College of Physicians Guideline for Low Back Pain (NCT05626049) |
Evaluate the effect of first-contact patient referral to physical therapists and doctors of chiropractic; determine if initial contact with these “primary spine practitioners” improves physical function, improves pain, and reduces opioid prescriptions in patients with a primary complaint of low back pain | Adults with low back pain in 3 academic healthcare systems | Cluster randomized trial |
| iPATH
Implementing Scalable, Patient-Centered Team-Based Care for Adults with Type 2 Diabetes and Health Disparities (NCT06251323) |
Refine and test an innovative practice transformation strategy to improve type 2 diabetes for NIH-designated priority populations | 12 clinics in federally qualified health centers in 4 regions | Stepped-wedge, cluster randomized, type 2 hybrid effectiveness-implementation trial |
| LungSMART
Population Health Management Approaches to Increase Lung Cancer Screening in Community Health Centers |
Test strategies to increase uptake of US Preventive Services Task Force–recommended lung cancer screening among patients in federally qualified health centers | Current and former smokers aged 50 to 80 years in community health centers in Utah | Individual-level randomization |
| MOMs Chat & Care Study
Maternal Outcomes Program: Testing Integrated Maternal Care Model Approaches to Reduce Disparities in Severe Maternal Morbidity (NCT06335381) |
Test the effectiveness of an integrated care model approach at 2 different levels of intensity designed to facilitate timely, appropriate care for high-risk Black and Hispanic birthing people and reduce risk for severe maternal morbidity | Black/African American and Hispanic pregnant adults at high risk for severe maternal morbidity in an obstetrics practice site | Individual-level randomization |
| NOHARM
Nonpharmacologic Options in Postoperative Hospital-based and Rehabilitation Pain Management (NCT04570371) |
Evaluate the feasibility of EHR-embedded patient- and clinician-facing decision support for nonpharmacologic pain care after surgery | Approximately 54,000 postoperative patients in 22 practice clusters in 4 large integrated healthcare systems | Cluster randomization by practice cluster |
| OPTIMUM
Group-Based Mindfulness for Patients With Chronic Low Back Pain in the Primary Care Setting (NCT04129450) |
Evaluate a group-based mindfulness program (mindfulness-based stress reduction) for patients with chronic low back pain within primary care | Approximately 450 patients with chronic low back pain in primary care clinics in 3 large healthcare systems | Individual-level randomization |
| RAMP
Reaching Rural Veterans: Applying Mind-Body Skills for Pain Using a Whole Health Telehealth Intervention (NCT06568250) |
Improve pain management and reduce opioid use among rural patients in the VA system | Veterans with chronic pain living in rural areas in the VA healthcare system | Type 2 hybrid effectiveness-implementation trial with individual-level randomization |
| STEP-2
Self-Testing for Cervical Cancer in Priority Populations |
Test the comparative effectiveness of in-clinic distribution of human papillomavirus self-sampling kits vs in-clinic plus mailed self-sampling kits or usual care, to improve cervical cancer screening rates | Patients in federally qualified health centers who are due or overdue for cervical cancer screening | Cluster randomization by clinic |
| TAICHIKNEE
Remote Tai Chi for Knee Osteoarthritis: An Embedded Pragmatic Trial (NCT06384898) |
Test a remote tai chi mind-body program in multiple healthcare systems’ outpatient practices using web-based technology, designed to improve patient centered outcomes of symptomatic knee osteoarthritis | Adults with a clinical diagnosis of knee osteoarthritis in 20 to 25 clinics in 4 healthcare systems in 4 geographic regions | Individually randomized group treatment trial |
Extending the Reach of the Embedded Pragmatic Trials Ecosystem
PCORnet
The National Patient-Centered Clinical Research Network (PCORnet) links multiple integrated healthcare systems and “patient-powered” networks to conduct comparative effectiveness research and explore questions about conditions, care, and outcomes that matter most to patients and their families. PCORnet consists of clinical data research networks and patient-powered clinical research networks that are linked through a distributed research network to facilitate multisite, observational, and interventional research (Fleurence et al 2014). The distributed research network harnesses data from EHRs for research, allows each participating organization to maintain physical and operational control over their data, and minimizes the transfer of individual-level clinical data (Fleurence et al 2014; Forrest et al 2021). PCORnet’s first pragmatic clinical trial was ADAPTABLE (Jones et al 2021).
Pain Management Collaboratory
The Pain Management Collaboratory (PMC) is jointly supported by the NIH, the Department of Defense, and the Department of Veterans Affairs. The program is developing the capacity to implement cost-effective, large-scale pragmatic clinical research in military and veteran healthcare delivery organizations, focusing on nonpharmacologic approaches to pain management and other comorbid conditions. The PMC supports 11 demonstration projects addressing such clinical areas as chronic low back pain, postoperative pain, and behavioral treatments for pain, among others.
National Institute on Aging (NIA) IMPACT Collaboratory
The NIA IMPACT Collaboratory aims to increase the nation’s capacity to conduct pragmatic clinical trials embedded within healthcare systems for people living with dementia and their caregivers. The NIA IMPACT Collaboratory is funding 1-year pilot studies that are meant to generate the preliminary data necessary to design and conduct full-scale embedded pragmatic trials that will be funded through other grant mechanisms such as the NIH or other sources.
Real-World Data and Real-World Evidence
We believe that when the term "real-world evidence" is used, the primary attribute that distinguishes it from other kinds of evidence is related to the context in which the evidence is gathered—in other words, in clinical care and home or community settings as opposed to research-intensive or academic environments. (Sherman et al 2016)
Embedded pragmatic trials can also be viewed in the context of discussions about real-world data and real-world evidence. Real-world data are data relating to patient health status or the delivery of healthcare routinely collected from a variety of sources, such as EHRs, claims and billing activities, product and disease registries, patient-generated data, and data gathered from sources that can inform health status (FDA). Real-world evidence is clinical evidence regarding the use and potential benefits or risks of a medical product derived from analysis of real-world data. Real-world evidence can be generated by different study designs or analyses, including but not limited to randomized trials, including large simple trials, pragmatic trials, and observational studies (prospective and/or retrospective).
- For more on the role of real-world data and real-world evidence in embedded pragmatic trials, read Real World Evidence: Mobile Health in the Living Textbook.
- In Advances at the Intersection of Digital Health, Electronic Health Records, and Pragmatic Clinical Trials: Real World Evidence: Contemporary Experience and Future Directions, a session of the Rethinking Clinical Trials Grand Rounds webinar series, a panel discusses how quality real-world evidence cannot be built without quality real-world data.
- In 2023 and 2024, the FDA issued 4 guidance documents for real-world data and real-world evidence intended to guide the selection and management of data sources to appropriately address study questions and support decision-making for drug and biological products. These guidance documents include:
- Real-World Data: Assessing Electronic Health Records and Medical Claims Data to Support Regulatory Decision-Making for Drug and Biological Products
- Data Standards for Drug and Biological Product Submissions Containing Real-World Data
- Real-World Data: Assessing Registries to Support Regulatory Decision-Making for Drug and Biological Products
- Considerations for the Use of Real-World Data and Real-World Evidence to Support Regulatory Decision-Making for Drug and Biological Products
John Concato, associate director for real-world evidence analytics with the FDA, discussed the FDA guidance in the June 24, 2022, session of the Rethinking Clinical Trials Grand Rounds, “FDA Draft Guidance on Real-World Evidence,” and the associated podcast episode.
SECTIONS
Resources
PCORnet Playbook
A guide to using PCORnet for research teams, patients and community partners, clinicians, and caregivers.

FDA Draft Guidance on Real-World Evidence; Rethinking Clinical Trials Grand Rounds; June 24, 2022
REFERENCES
Califf RM, Sugarman J. 2015. Exploring the ethical and regulatory issues in pragmatic clinical trials. Clin Trials. 12:436–441. doi:10.1177/1740774515598334. PMID: 26374676.
Coronado GD, Petrik AF, Vollmer WM, et al. 2018. Effectiveness of a mailed colorectal cancer screening outreach program in community health clinics: The STOP CRC cluster randomized clinical trial. JAMA Intern Med. 178(9):1174-1181. doi: 10.1001/jamainternmed.2018.3629. PMID: 30083752.
DeBar L, Mayhew M, Benes L, et al. 2022. A primary care-based cognitive behavioral therapy intervention for long-term opioid users with chronic pain : A randomized pragmatic trial. Ann Intern Med. 175(1):46-55. doi: 10.7326/M21-1436. PMID: 34724405.
Dember LM, Lacson E Jr, Brunelli SM, et al. 2019. The TiME trial: A fully embedded, cluster-randomized, pragmatic trial of hemodialysis session duration. J Am Soc Nephrol. 30(5):890-903. doi: 10.1681/ASN.2018090945. PMID: 31000566.
Fleurence RL, Curtis LH, Califf RM, Platt R, Selby JV, Brown JS. 2014. Launching PCORnet, a national patient-centered clinical research network. J Am Med Inform Assoc. 21:578–582. doi:10.1136/amiajnl-2014-002747. PMID: 24821743.
Forrest CB, McTigue KM, Hernandez AF, et al. 2021. PCORnet® 2020: current state, accomplishments, and future directions. J Clin Epidemiol. 129:60-67. doi: 10.1016/j.jclinepi.2020.09.036. PMID: 33002635.
Gohil SK, Septimus E, Kleinman K, et al. 2025a. Improving empiric antibiotic selection for patients hospitalized with abdominal infection: The INSPIRE 4 cluster randomized clinical trial. JAMA Surg. 160(7):733-743. doi: 10.1001/jamasurg.2025.1108. PMID: 40208583.
Gohil SK, Septimus E, Kleinman K, et al. 2025b. Improving empiric antibiotic selection for patients hospitalized with skin and soft tissue infection: The INSPIRE 3 Skin and Soft Tissue randomized clinical trial. JAMA Intern Med. 185(6):680-691. doi: 10.1001/jamainternmed.2025.0887. PMID: 40208610.
Grudzen CR, Siman N, Cuthel AM, et al. 2025. Palliative care initiated in the emergency department: A cluster randomized clinical trial. JAMA. 333(7):599-608. doi: 10.1001/jama.2024.23696. PMID: 39813042.
Ho PM, Glorioso TJ, Allen LA, et al. 2025. Personalized patient data and behavioral nudges to improve adherence to chronic cardiovascular medications: A randomized pragmatic trial. JAMA. 333(1):49-59. doi: 10.1001/jama.2024.21739. PMID: 39621340.
Huang SS, Septimus E, Kleinman K, et al. 2019. Chlorhexidine versus routine bathing to prevent multidrug-resistant organisms and all-cause bloodstream infections in general medical and surgical units (ABATE Infection trial): A cluster-randomised trial. Lancet. 393(10177):1205-1215. doi: 10.1016/S0140-6736(18)32593-5. PMID: 30850112.
Jarvik JG, Meier EN, James KT, et al. 2020. The effect of including benchmark prevalence data of common imaging findings in spine image reports on health care utilization among adults undergoing spine imaging: A stepped-wedge randomized clinical trial. JAMA Netw Open. 3(9):e2015713. doi: 10.1001/jamanetworkopen.2020.15713. PMID: 32886121.
Jones WS, Mulder H, Wruck LM, et al. 2021. Comparative effectiveness of aspirin dosing in cardiovascular disease. N Engl J Med. 384:1981-1990. doi: 10.1056/NEJMoa2102137. PMID: 33999548.
Melnick ER, Nath B, Dziura JD, et al. 2022. User centered clinical decision support to implement initiation of buprenorphine for opioid use disorder in the emergency department: EMBED pragmatic cluster randomized controlled trial. BMJ. 377:e069271. doi: 10.1136/bmj-2021-069271. PMID: 35760423.
Mitchell SL, Volandes AE, Gutman R, et al. 2020. Advance care planning video intervention among long-stay nursing home residents: A pragmatic cluster randomized clinical trial. JAMA Intern Med. 180(8):1070-1078. doi: 10.1001/jamainternmed.2020.2366. PMID: 32628258.
Platt R, Bosworth HB, Simon GE. 2024. Making pragmatic clinical trials more pragmatic. JAMA. 332:1875-1876. doi: 10.1001/jama.2024.19528. PMID: 39356531.
Sherman RE, Anderson SA, Dal Pan GJ, et al. 2016. Real-World Evidence - What Is It and What Can It Tell Us? N Engl J Med. 375:2293-2297. doi:10.1056/NEJMsb1609216. PMID: 27959688.
Simon GE, Shortreed SM, Rossom RC, et al. 2022. Effect of offering care management or online dialectical behavior therapy skills training vs usual care on self-harm among adult outpatients with suicidal ideation: A randomized clinical trial. JAMA. 327(7):630-638. doi: 10.1001/jama.2022.0423. PMID: 35166800.
Thorpe KE, Zwarenstein M, Oxman AD, et al. 2009. A pragmatic-explanatory continuum indicator summary (PRECIS): a tool to help trial designers. J Clin Epidemiol. 62:464–475. doi:10.1016/j.jclinepi.2008.12.011. PMID: 19348971.
Vazquez MA, Oliver G, Amarasingham R, et al. 2024. Pragmatic trial of hospitalization rate in chronic kidney disease. N Engl J Med. 390(13):1196-1206. doi: 10.1056/NEJMoa2311708. PMID: 38598574.
Volandes AE, Chang Y, Lakin JR, et al. 2025. An intervention to increase advance care planning among older adults with advanced cancer: A randomized clinical trial. JAMA Netw Open. 8(5):e259150. doi: 10.1001/jamanetworkopen.2025.9150. PMID: 40343696.
Zatzick D, Jurkovich G, Heagerty P, et al. 2021. Stepped collaborative care targeting posttraumatic stress disorder symptoms and comorbidity for US trauma care systems: A randomized clinical trial. JAMA Surg. 156(5):430-474. doi: 10.1001/jamasurg.2021.0131. doi: 10.1001/jamasurg.2021.6534. PMID: 33688908.
ACKNOWLEDGMENTS
Contributing editors of previous versions of this chapter include Jonathan McCall, Karen Staman, and Liz Wing of the NIH Pragmatic Trials Collaboratory Coordinating Center.



